Pregnancy is often seen as one of the most important and delicate times in a woman’s life. Across cultures and countries, it is a period when families become extra careful - choosing foods thoughtfully, planning regular antenatal visits, and avoiding anything that might put the baby at risk. Every small decision feels significant, because two lives are intertwined in it.
In recent years, one simple yet powerful act has quietly become part of this circle of care: vaccination during pregnancy. More than just protecting the mother, these vaccines help build a shield around the baby - before birth, at birth, and in the first vulnerable months of life.
Maternal Vaccination: A Proven Strategy
Newborns have immature immune systems and limited ability to fight infections. Some of the most dangerous infections in early infancy such as tetanus, influenza, pertussis, and Respiratory Syncytial Virus (RSV), either cannot be fully prevented by vaccination at birth or cause severe disease before routine immunization schedules take effect. Maternal vaccination elegantly bridges this gap. It does not replace infant vaccination; it complements it by providing protection during the most critical early window of life. The logic is simple but powerful: protect the mother, and you protect the baby.
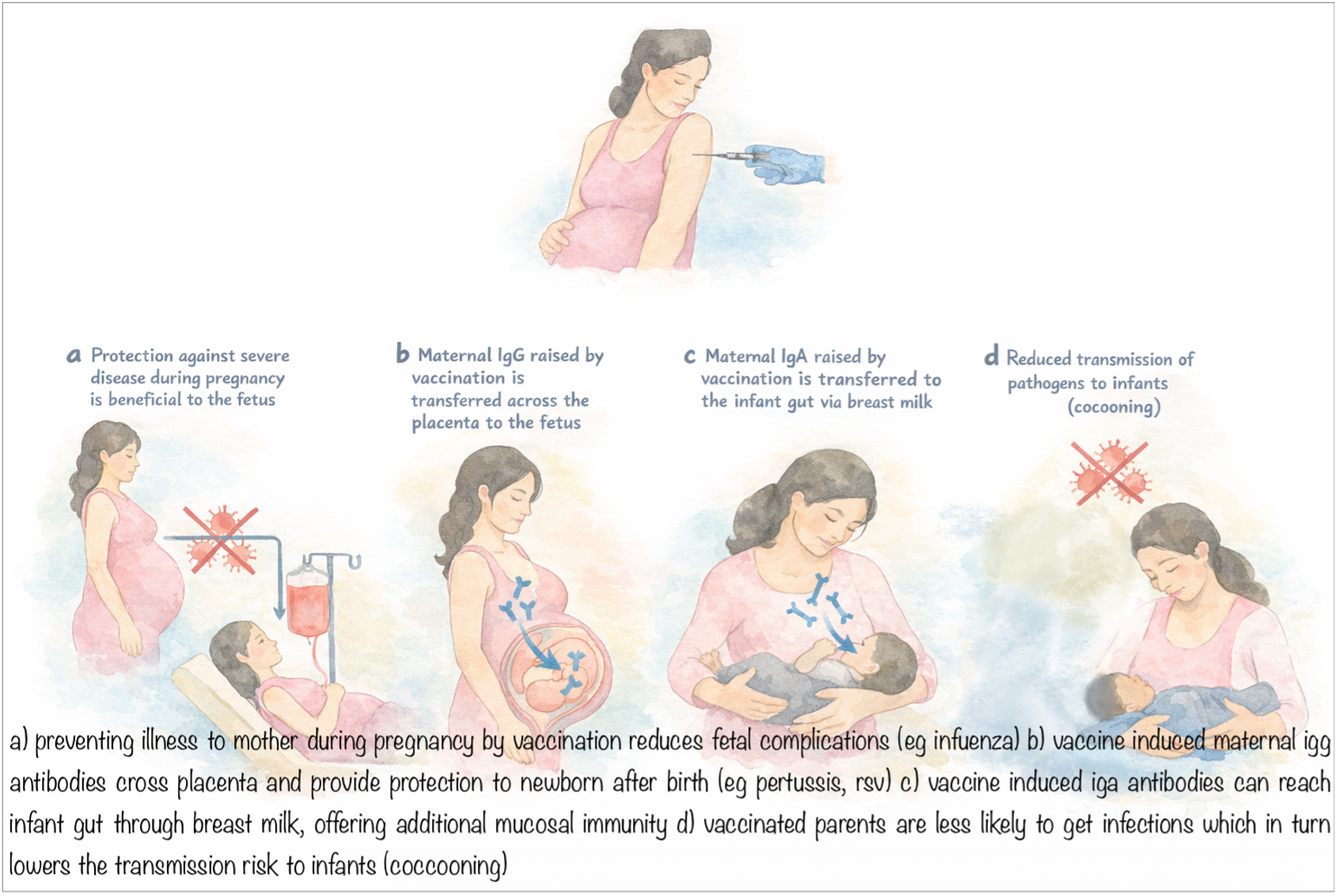
Think of maternal vaccination as building a protective bubble around a baby; starting in the womb and extending into the first months of life. From shielding the mother during pregnancy, to passing antibodies through the placenta and breast milk, and even reducing the risk of infection in the household, maternal vaccination creates multiple layers of defense around the baby. The figure below shows how these different protective mechanisms work together to protect the baby (1).
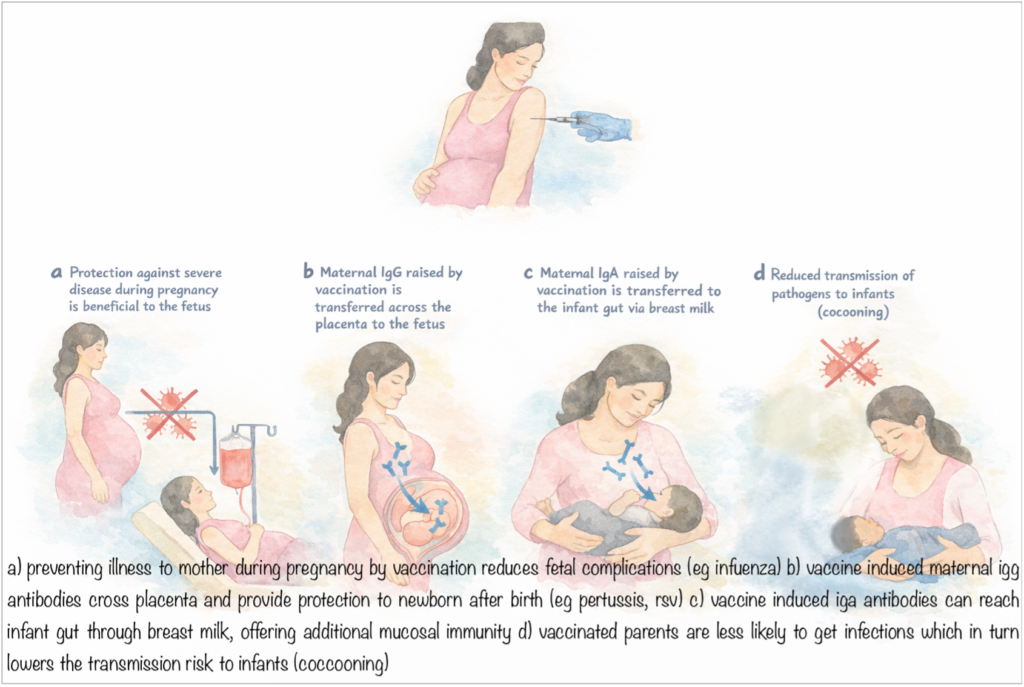
The Success of Maternal Vaccination
Maternal tetanus vaccination stands as one of the great success stories of public health. Through the Maternal and Neonatal Tetanus Elimination (MNTE) initiative, deaths from neonatal tetanus have fallen dramatically from an estimated 200,000 in 2000 to about 24,000 in 2021, an 88% reduction and as of 2024, only 10 countries have yet to achieve elimination (2). This progress has been driven by a combination of strategies, including strengthening routine immunization of pregnant women, targeted vaccination campaigns in high-risk areas, promotion of clean deliveries, and improved surveillance, with vaccination remaining the cornerstone, especially in low- and middle-income countries where unsafe delivery practices and limited access to care persist. Similar success has been seen with maternal vaccination against pertussis and influenza, which has protected countless young infants during their most vulnerable months.
Why This Matters for Global Health
Maternal vaccination is more than a biomedical intervention; it is a health systems strategy.
In many countries, antenatal care coverage is higher than postnatal or early infancy care. This makes pregnancy a unique and powerful opportunity to deliver life-saving interventions. From a programmatic perspective, maternal vaccination also strengthens the value of antenatal care and reinforces trust in health systems.
The experiences have taught important lessons:
- Maternal vaccines can be safely delivered through routine antenatal care.
- They can achieve high coverage when integrated into existing health systems.
- And when well-communicated, they are widely accepted by pregnant women and families.
Challenges That Must Be Addressed
Despite its promise, maternal immunization is not without challenges.
- Clear communication is essential. A pregnant woman’s decision to get vaccinated often comes down to a few simple factors: trust in the vaccine, a clear recommendation from her healthcare provider, and easy access during routine antenatal visits. Pregnant women and families must understand why vaccines are recommended and how they protect both mother and child. Healthcare workers need training and confidence to counsel effectively.
- As new maternal vaccines move closer to introduction, surveillance systems must be strengthened to better define disease burden and measure vaccine impact. Countries will also need clear guidance on prioritization, delivery strategies, and sustainable financing to ensure these vaccines are implemented effectively and at scale.
- Equity is perhaps the biggest concern. Those at greatest risk of early-life infections must not be the last to benefit. Maternal vaccines should be part of universal immunization programs and provided free of cost, so that protection reaches those who need it most.
Looking Ahead
Maternal vaccination represents one of the most powerful ideas in prevention: one intervention, two lives protected.
With the expansion of the maternal immunization portfolio, the coming decade presents a significant opportunity to further reduce early-life morbidity and mortality globally. Vaccines against tetanus, influenza, and pertussis have already demonstrated substantial public health impact. In addition, vaccines targeting respiratory syncytial virus and group B Streptococcus are now in advanced stages of development or early implementation, reinforcing maternal immunization as a robust platform for protecting mothers and young infants against multiple serious infections.
In the quiet space between pregnancy and birth, maternal vaccination is helping rewrite the story of vulnerability into one of protection.
Written by ISID Emerging Leader, Dr. Tintu Varghese